What do we know so far about airborne transmission and how does it differ from respiratory droplet transmission?

Last modified on Feb. 17, 2021
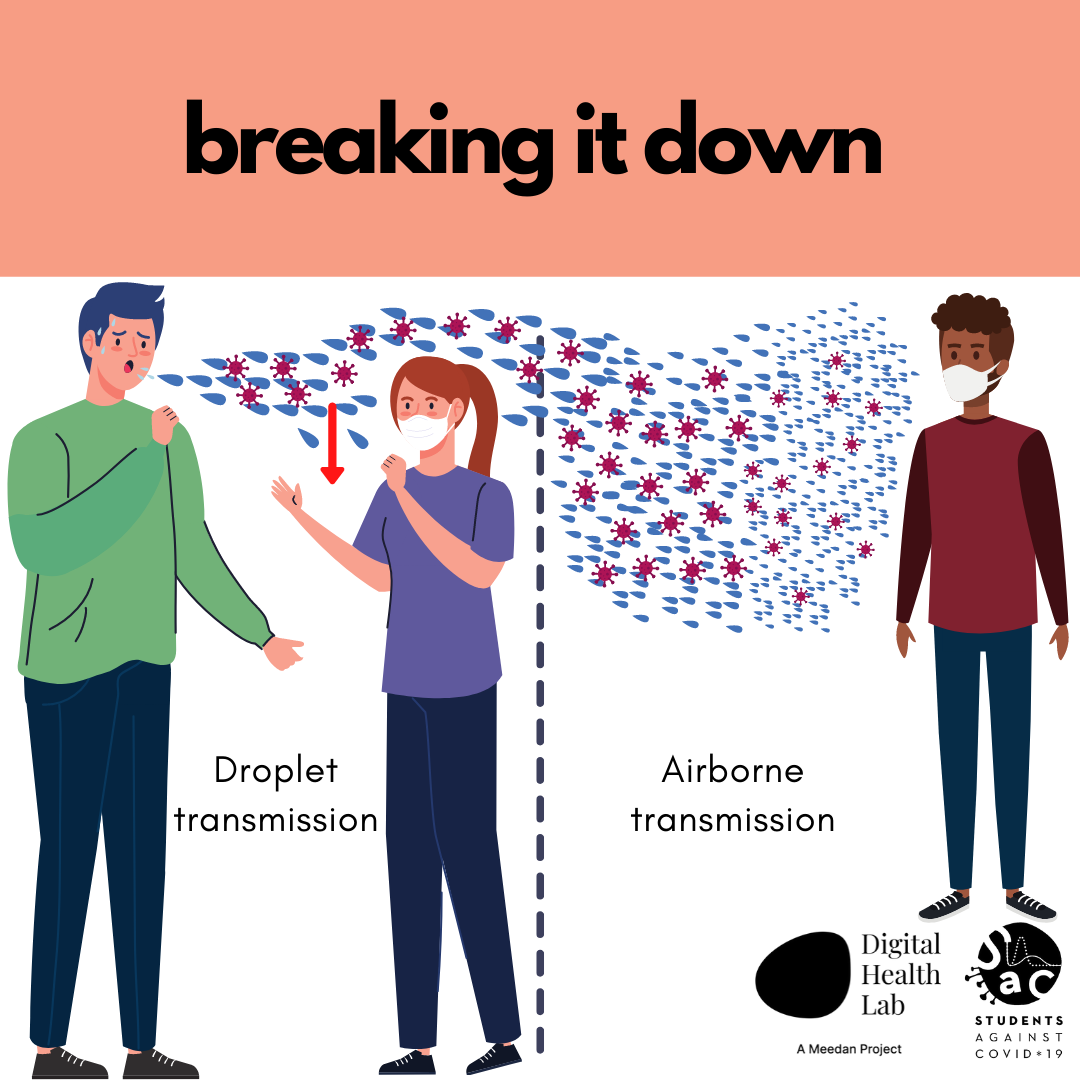
There is increasing evidence that COVID-19 can spread through airborne transmission, which is when a person infected with COVID-19 releases tiny droplets of fluid into the air called ‘droplet nuclei’ by coughing, sneezing, talking, or during some medical appointments and procedures. Droplet nuclei are very light, relatively dry, and microscopic in size so they can remain suspended in the air like a mist, which is why airborne transmission is also called ‘aerosol transmission.’
This is different from the main theory that the virus spreads through bigger respiratory droplets that are heavier, fall to the ground relatively quickly, and do not remain suspended in the air or spread through the air.
While researchers are continuing to study aerosol transmission of COVID-19, the World Health Organization (WHO) and the U.S. Centers for Disease Control and Prevention (CDC) acknowledged evidence of airborne transmission in poorly ventilated spaces. Enclosed spaces have been found—through scientific studies as well as case studies—to contain enough virus to cause infections in people more than six feet apart, or who passed through a space soon after an infectious person left the room.
One study conducted at the University of Nebraska Medical Center collected air and surface samples from the rooms of isolated individuals to examine viral shedding, and found evidence of the novel coronavirus in the air from isolated individuals who had COVID-19 (including at a distance from the infected individual and outside of their room in the hallway).
As a second piece of evidence, a study from Singapore found that COVID-19 virus aerosol particles were found in two “airborne infection isolation rooms” in hospital wards, despite these rooms being intentionally well ventilated to prevent transmission.

In a study that modeled the transmission of COVID-19 during the outbreak on the Diamond Princess cruise ship in early 2020, researchers found that aerosol inhalation of the virus was likely the dominant contributor to COVID-19 transmission among passengers.

Another study outlined the case of the Skagit Valley Chorale rehearsal in Mount Vernon, Washington, which took place in early March 2020 and resulted in 45 out of 60 members of the chorus testing positive for or showing COVID-19 symptoms after a 2 ½ hour indoor practice session. No attendees reported physical contact between members, as person-to-person contact and touching of surfaces was intentionally limited. No one was located within 3 meters in front of the index COVID-19 case, where larger respiratory droplets from that individual would have likely landed.
The authors concluded that inhalation of infectious respiratory aerosol from shared air was the leading mode of transmission and that dense occupancy, long duration, loud vocalization, and poor ventilation increased risk.
Another case study was reported in China in early February when a who passed by the door of a symptomatic patient several times person contracted COVID-19.
Finally, one China-based study compared risks of COVID-19 outbreak among 126 passengers taking two buses on a 100-minute round trip. Compared to individuals in the non-exposed bus (Bus #1), those in the exposed bus (Bus #2) were 41.5 times more likely to be infected, suggesting airborne transmission of the virus, particularly given the closed environment with air recirculation and lack of contact between passengers.

These studies, and others like them, highlight the importance of combining proper ventilation with cloth masks and social distancing to prevent transmission of the virus. The U.S. CDC’s most recent guidelines suggest wearing a cloth mask over a surgical mask or an individual KN95/N95 mask as these methods can offer the most protection from the virus, but any mask offers substantially more protection than not wearing one. Studies such as these are particularly important as it would not be ethical to run a randomized control trial (RCT) to test different transmission modes in infecting individuals, and given that it’s difficult to specifically pinpoint in a study how someone was infected without a highly controlled environment, such as that of an RCT.
Public health experts have repeatedly warned that airborne transmission is most likely contributing to transmission, especially in indoor spaces, and recommendations should incorporate the need for sufficient ventilation, high-efficiency filtration, and limiting crowded spaces, in addition to universal adoption of masks, social distancing, and frequent handwashing with soap and water.
Context and background
Respiratory droplet transmission happens when disease, in this case COVID-19, spreads through droplets expelled by an infected person, through coughing, sneezing, talking, or even just breathing; these droplets are larger than 5-10 micrometers. One micrometer is one millionth of a meter. Respiratory droplets are relatively heavy, and fall to the ground quickly. In contrast, airborne transmission is when residue from droplets smaller than 5 micrometers, or dust particles carrying the virus, stay suspended in the air for a while and travel as their air moves. Scientists and the World Health Organization (WHO) have recognized that evidence is emerging on the possibility of airborne transmission, particularly in crowded, closed, poorly ventilated settings.
If airborne transmission of COVID-19 is significant, this has major implications for containment efforts (ex. masks may be needed indoors and even in socially-distant settings, ventilation systems may need to minimize recirculating air and find ways to filter or disinfect contaminated air, etc.).
The US CDC has recently acknowledged well-documented evidence of airborne transmission of SARS-CoV-2 under circumstances of enclosed spaces, prolonged exposure to respiratory particles from an infectious person, or inadequate ventilation.
Used with permission by Health Desk, a public health hub that explains emerging COVID-19 science.


